I am a Catholic Deacon and also a hospital chaplain. I work in a secular hospital, not a religious one. My hospital is in Tucson, Arizona. As I write this, Tucson, Arizona is in the epicenter of the global COVID-19 virus. As I write this, 7 of our 10 units are either fully occupied with COVID-19 patients or partially. This is a reflection on life at Ground Zero in the COVID-19 Pandemic.
Beginning Of The Day
I walk into the office before dawn. Put my lunch in the refrigerator, hang my change of clothes on the back of the door and pick up the morning report on the printer.
Entering my office, I put my things down on my desk, pick up my work phone and go the front office printer where I pick up my intra-hospital pager and grab the stack of requests for a chaplain visit for the day, glancing them over for any STAT requests. Seeing none, I put them on the desk, and head to the one of the units to attend the morning ‘huddle’ with the nurses and patient care techs.
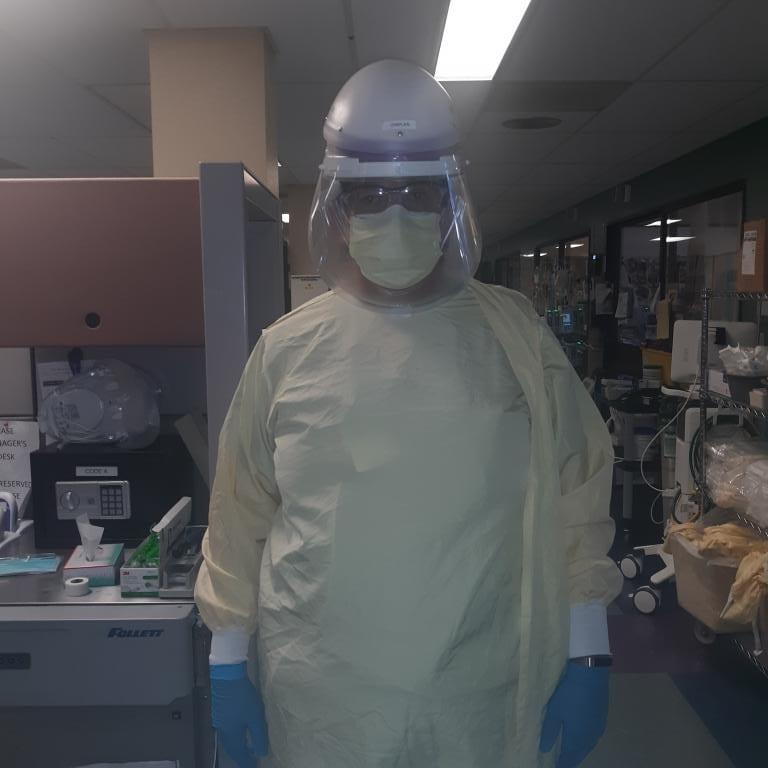
It Begins
I enter the staff lounge for the huddle, and my phone alert sounds a text. It turns out I am needed in another unit STAT for the family of a dying patient.
I quickly leave and hurry down the hallway to the requesting unit, find the attending nurse, get a one-minute update on the situation, open the medical record and do an additional minute of review, looking for pertinent facts; religious preference, patient name, family member’s names. I enter the room and introduce myself, trying to quickly assess what is happening in front of me and how I can assist them.
The religious preference was not listed in the medical record for some unknown reason. They do not share my personal faith. I ascertain their religious support system – are they affiliated with a particular faith group / church / congregation?
Providing Comfort
I am searching for vital clues on how they relate to the mystical life. My faith, my personal prayers may be helpful, but it may be of no comfort. I have to find their comfort spot, their pathway and I have scant minutes to do so.
The spouse tells me of their life together as the patient has lost the capacity to speak, to motion or even to open their eyes. After a few minutes I have the information I seek and invite them to place themselves in the presence of a power greater than they or I. We offer invocations of peace and safe passage, of being reunited one day and of living again without pain or suffering.
Within 30 minutes, it is done. I offer support and prayers for the spouse and invite them to spend the last minutes of their life together recalling the love, the good times, the favorite memories and to give the gift of forgiveness to their spouse for anything that they have left unsaid, undone or incomplete.
I leave the room, shutting the door softly behind me, and I return to the unit where I started. Speaking to the charge nurse, I get an overview of the unit – progress of the patients, expected events, things to watch for and most importantly who may need assistance, (both patient and staff). I return to the office and pick up the stack of orders I left there almost an hour ago.
The second chaplain has just returned from a similar liaison with another unit in the hospital. Over a cup of tea, we quickly compare notes, searching for common concerns and dividing up the stack of orders. Lists and a plan are printed, checked and reviewed and we head out.
The First COVID Patient
I approach the first room on my list and prepare to enter. This is a COVID-19 room. Gown, shoe covers, hair cover, gloves, isolation helmet with positive air flow (Papair) and after 5 minutes of getting ready, I finally enter the first room on my list.
Approaching the person in the bed, I introduce myself and ask how I can assist them. Listening carefully to their concern and worry about being admitted to the hospital in a COVID-19 room, I start the search for spiritual clues again.
This patient is Baptist, and they ask me why God hates them, how did their faith fail and cause them to contract this virus? Wasn’t God supposed to protect them if they had faith? They tell me they feel like Job. They ask for prayer.

My natural tendency to grasp their hands as we pray has to be held back as they are in an infectious state. Even with gloves, the human touch of one hand to another is minimized to help control the spread of this unwanted intruder into the norm of life. Again, I invite them to place themselves in the presence of the divine and express the groans of their soul to the Father.
They say thank you and I prepare to leave the room. Stopping at the door, I remove the shoe covers first, then the gown and lastly the gloves, leaving the hair net and protective air helmet on until outside. Once outside, I find the bleach wipes and wipe the outside surfaces of the helmet, the face shield, the chin guard and then shut the air flow off, loosen the head band and remove the helmet.
I take the hairnet off and throw it in the trash, wipe my shoes with the bleach wipe, and then my hands and throw it away too. I find a chair nearby, sit down and make my notes for the patient’s chart. Sometimes I get to do this right after I see the person. Other times I have to make hieroglyphic like notes to enter into the chart later.
Another COVID Patient
I glance at my list and start toward the second patient. The overhead page, and my phone both erupt with the announcement of a Code Blue in one of the units. I pick up my step and head there. I arrive at the same time as my partner and we quickly decide who will handle it.
This time, it is me. I look up the patient in the computer, find the demographic information such as spouse and spouse phone number. Is there a living will or advance directives? What is their religious preference? This patient is Jewish. The spouse has not been called yet to let them know what is happening.
I speak with the House Supervisor and stand by near the door to the room. Should things not go well I am ready to enter. Oh wait, this too is a COVID-19 patient. I repeat the dressing drill I just did a few minutes earlier – shoe cover, hair cover, gown, gloves but I do not put on the helmet – yet.
I catch the eye of the doctor directing the code and get an indication of how it is going. Not getting a good indication, I open my book of prayer and scripture and find the Psalms. The house supervisor motions to me to join her and hands me the phone. I speak to the spouse to provide comfort and prayer and find out what their faith life is like.
A Busy Two Hours
As it turns out, after 45 minutes, this one ends well. After the code team leaves, I enter the room and recite some Psalms. Repeating the dance of the exit, I remove each piece of protective gear in order again. I make my notes and return to my list and I never got to the second person on my list. I have been on the floor for a little over two hours now.
Part two of the reflection will be posted tomorrow.
About Our Guest Blogger
Deacon Andy Corder is a Deacon in the Diocese of Tucson. He is a hospital chaplain in one of the largest hospitals in Tucson, AZ. This is part one of a reflection that will be presented in three parts.













