WILLS POINT, TX – Gospel for Asia (GFA World) founded by Dr. K.P. Yohannan issues an extensive Special Report on the deadly diseases brought by the mosquito and the storied impact of faith-based organizations on world health, fighting for the Kingdom to “come on earth as it is in heaven.”
This is Part Two of a Three-Part Series on FBO Initiatives to Combat Malaria and Other World Health Concerns. Go here to read Part 1 and Part 3.
Faith-Based Organizations as Seen Through the Bite of the Mosquito
Let’s look at that mosquito again, the anopheles that carries some form of the genus Plasmodium, which is the genesis of several strains of potentially deadly malaria parasites. In addition to malaria, the bite of various mosquitoes can also transmit dengue and yellow fever as well as the Zika, West Nile and African Sleeping Sickness viruses. The long battle against the lone mosquito multiplied by millions of its kind presents a simulacrum through which an enormous topic—modern medicine outreaches as influenced by faith—can be viewed.
 One of the specific health ministries Gospel for Asia (GFA) initiated in 2016 was to participate in World Mosquito Day, observed every August 20 to raise awareness about the deadly impact of mosquitoes. This global initiative encourages local governments to help control malaria outbreaks, and it also raises funds from large donor organizations and national governments to underwrite worldwide eradication efforts. Discovering and applying means of mosquito control in overpopulated areas of the world is essential, but the task is so large and the enemy so canny that planners have discovered they must rely on a combination of efforts that activate local communities and the leaders in those communities, non-governmental organizations (NGOs), faith-based organizations (FBOs) and faith-based development organizations (FBDOs).
One of the specific health ministries Gospel for Asia (GFA) initiated in 2016 was to participate in World Mosquito Day, observed every August 20 to raise awareness about the deadly impact of mosquitoes. This global initiative encourages local governments to help control malaria outbreaks, and it also raises funds from large donor organizations and national governments to underwrite worldwide eradication efforts. Discovering and applying means of mosquito control in overpopulated areas of the world is essential, but the task is so large and the enemy so canny that planners have discovered they must rely on a combination of efforts that activate local communities and the leaders in those communities, non-governmental organizations (NGOs), faith-based organizations (FBOs) and faith-based development organizations (FBDOs).
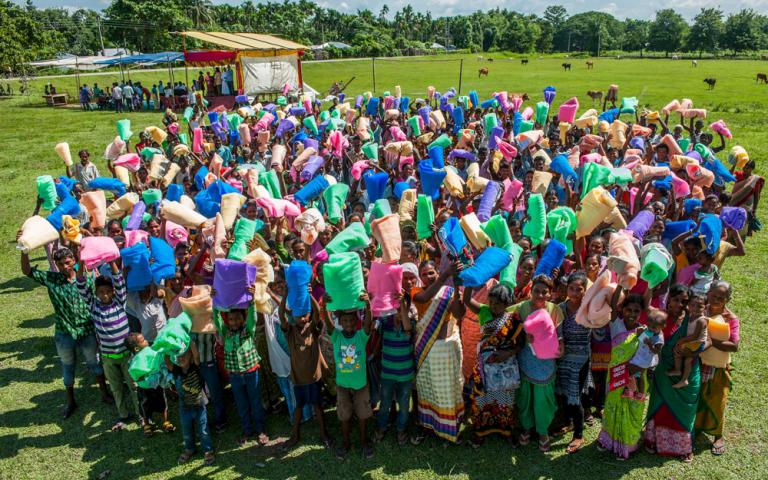
In 2016, workers collaborating with Gospel for Asia (GFA) distributed some 600,000 mosquito nets, many of which were given to people living in districts where there are high malaria risks and high poverty levels. Due to poverty, these folks were unable to procure the simplest of means to prevent mosquito-borne diseases. In addition to the nets, which were given away without charge, Gospel for Asia (GFA) conducted disease-awareness training in order to heighten understanding about preventive measures.
[su_qoute]In the majority of rural areas, there are no clinics, no hospitals, no medical professionals and no treatment protocols.[/su_quote]This effort was compatible with the movement back to a primary health care emphasis as delineated in the 1978 Alma-Ata Declaration encouraged by the World Health Organization, which proclaimed the principles of what was meant by the concept of primary health care and the overreaching need for it. While a few populations in developing countries have access to tertiary health care—hospitals and clinics and professionals trained in medical schools, drugs and diagnostic equipment—the vast majority of the rest of the populace can access extremely limited or next-to-no available health care. In the majority of rural areas, for instance, there are no clinics, no hospitals, no medical professionals and no treatment protocols. (This medical desert is also becoming a problem in the United States; as rural populations shrink, hospitals and clinics cannot afford to stay open.)
The Alma-Ata conference recommended a redirection of approaches to what is termed primary health care. Charles Elliott, an Anglican priest and development economist, summarized the suggested changes as follows:
- An increasing reliance on paraprofessionals (often referred to as community health workers) as frontline care givers;
- The addition of preventive medicine to curative approaches;
- A noticeable shift from vertical, disease-specific global health initiatives to integrated, intersectoral programs;
- A willingness to challenge the dominant cost-effectiveness of analysis, particularly as it was used to justify a disproportionate distribution of health care resources for urban areas; and
- A heightened sensitivity to the practices of traditional healing as complementary rather than contradictory to the dominant Western medical model.
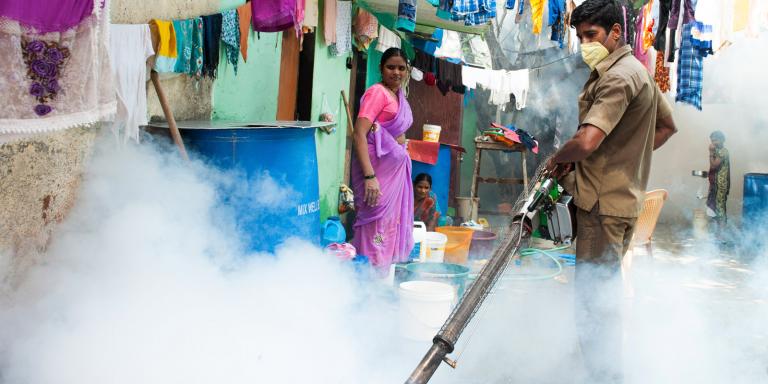
India’s Progress in Combating Malaria
In 2015, the World Health Organization set a goal of a 40 percent reduction in malaria cases and deaths by 2020 and estimated that by that deadline, malaria could be eradicated in 11 countries. The first data reports were extremely encouraging, but attrition began to set in, due to what experts feel is a lag in the billions of donor funds needed to combat the disease. The 2018 World Malaria Report health data now indicate a slowing in the elimination of the disease and even growth in disease incidents and deaths. This slide is disheartening to world health officials, particularly since early reports gave evidence of real impact against morbidity.
India, however, according to the 2018 report, is making substantial progress: “Of the 11 highest burden countries worldwide, India is the only one to have recorded a substantial decline in malaria cases in 2017.”
The report goes on to state that the country, which accounted for some 4 percent of global malaria cases, registered a 24 percent reduction in cases over 2016. The country’s emphasis has been to focus on the highly malarious state of Odisha. The successful efforts were attributed to a renewed government emphasis with increased domestic funding, the network of Accredited Social Health Activists (ASHAs)—an intended 900,000 women assigned to every village with a population of at least 1,000—and strengthened technological tracking, which allowed for a focus on the right mix of control measures. The aim of India’s National Vector Borne Disease Control Programme is the eradication of malaria.
Remember the ever-present mosquito? Studies conducted by WHO released the findings of a major five-year evaluation reporting that people who slept under long-lasting insecticidal nets had significantly lower rates of malaria infection than those who did not use a net.
In coordination with this national effort, Gospel for Asia (GFA)-supported workers distributed nets to villagers, in student hostels, among workers in the tea-growing district of Assam and many other areas while at the same time leading disease-awareness programs to tea-garden employees.

Imagine a dusty village filled with women wearing vibrant-colored clothing. Little children dance around or stand intrigued, their huge brown eyes open. Nets are placed into outstretched hands. Women smile; gifts are always appreciated. Men listen carefully to the reasons why bed nets are essential and why it is necessary to spray the home and rooms. People bow their heads; they raise pressed hands to their faces. “Namaste,” they say giving thanks.
Envision a room at night with six to eight buzzing, dive-bombing mosquitoes and give thanks that there are organizations around the world that pass out the free gift of bed nets that not only keep humans from being stung but also prevent them from becoming wretchedly ill.
Historical Cooperation
The possibility of eradicating malaria rests in the efforts of Dr. Ronald Ross, born in Almora, India, in 1857 to Sir C.C.G. Ross, a Scotsman who became a general in the Indian Army. Reluctant to go into medicine, the son nevertheless bowed to his father’s wishes to enter the Indian Medical Service.
At first, Ross was unconvinced that mosquitoes could possibly be carriers of malaria bacteria, yet his painstaking, mostly underfunded laboratory discoveries eventually convinced him that the hypothesis of a mentor, Patrick Manson, an early proponent of the mosquito-borne malaria theory, was correct. (Manson is also considered by many to be the father of tropical medicine.) Another contemporary, the French Army doctor Alphonse Laveran, while serving at a military hospital in Algeria, had observed and identified the presence of parasitic protozoans as causative agents of infectious diseases such as malaria and African Sleeping Sickness.

On August 20, 1897, in Secunderabad, Ross made his landmark discovery: the presence of the malaria parasite in humans carried by the bite of infected mosquitoes. (For obvious reasons, Ross was also the founder of World Mosquito Day.) Disease can’t be combated unless its source is identified, nor can it be optimally controlled. Certainly, without this knowledge, it can’t be eradicated. In 1902, Ronald Ross was awarded the Nobel Prize in Medicine.
Here again, through the bite of the mosquito, we see the collaborative effort that undergirds progress. Three doctors intrigued with conquering the morbidity of disease take painstaking efforts to prove their theories, and each one builds on the discoveries of the other, with eventual dramatic results.

Change Involves Everyone
Progress is not possible without collaborative work. Statisticians, medical teams and universities, as well as local village training centers, governments of developing countries and local leadership in towns and cities must all work together. The job requires donations from wealthy donor nations as well as from national local budgets. We need the skills of technological gurus, engineers and the extraordinary capabilities of highly trained health care professionals and sociologists. In addition, we also need the involvement of those who care about the soul of humans and who have insisted, because their lives are driven and informed by a compassionate theology, that every human is made in the image of God.
Gospel for Asia (GFA), through its mosquito net distribution—and its many other ministries—stands central in the contemporary initiatives of health-based, community-centered, preventive health care.
These are some of the strategic players who must all be involved, and stay involved, if the MDGs, now the Millennium Sustainable Development Goals, are to be reached.
This model of interactivity, whether present-day players realize it or not, intriguingly stems from a decades-old initiative stimulated by the World Council of Churches (WCC) in the last century, based in a carefully crafted theological understanding by the Christian Medical Commission (CMC), which concurrently and cooperatively developed the meaning of health that simultaneously contributed to the WHO’s significant 1978 Declaration of Alma-Ata. This resulted in a focus on primary care as a more just and egalitarian way to distribute resources in order to treat a larger proportion of the world’s population.

This forgotten story needs to be resurrected because it demonstrates the power of intentional intersectoral cooperation between secular and religious health outreaches. It also exemplifies a more holistic redefinition of the meaning of health that has the potential to positively impact disease-ridden environments in the many populations that are generally minimally treated or completely untreated in developing countries. In a day when Western technologically centered medicine, driven by what some in health communities are starting to call the “industrial medical complex,” is beginning to wane in its understanding of the meaning of superior patient-centered care, this model needs to be adapted to what we think of as the more sophisticated treatment approaches in health care.
Our Friends, the Critics (Because Their Criticism Makes Us Think)
Let’s first take a quick look at what critics of faith-based medical outreaches have to say. Instead of delving into the academic literature, which though informative often provides a tedious plod through footnotes and specialized terminology, let’s look at the growing field of “opinion” journalism.

After the 2014 Ebola outbreak in Liberia, Africa, an article appeared in Slate Magazine by Brian Palmer, a journalist who covers science and medicine for the online magazine. This periodical represents an admittedly liberal perspective, and that bias, though the author attempts to play fair, is shown even in the headline to his report: In Medicine We Trust: Should we worry that so many of the doctors treating Ebola in Africa are missionaries?” Great lead line; it certainly caught the attention of my friends and colleagues who work in medical missions.
Palmer summarizes his basic critique in this paragraph: “There are a few legitimate reasons to question the missionary model, starting with the troubling lack of data in missionary medicine. When I write about medical issues, I usually spend hours scouring PubMed, a research publications database from the National Institutes of Health, for data to support my story. You can’t do that with missionary work, because few organizations produce the kind of rigorous, peer-reviewed data that is required in the age of evidence-based medicine.”
Although PubMed is a worthy venue for medical specialists as well as the generalist writing in the field—with some 5.3 million archived articles on medical and health-related topics—it alone may be a truncated resource for the kind of information that could have more richly framed this article. Interviews with at least a few boots-on-the-ground, living faith-based medical professionals who have given their lives to wrestling with the health care needs in countries far afield from Western medical resources, might also have been a better means of achieving a professional journalistic approach. In addition, there is a whole body of evidence-based research that a superficial treatment such as this did not access.

Sharon Bieber of Medical Ambassadors International responds to the Slate article out of a lifetime of framing health care systems with her husband, Dr. Bill Bieber, in mostly underdeveloped nations in the world. It is important to note the Canadian government awarded these “medical missionary types” the Meritorious Service Medal—an award established by Her Majesty Queen Elizabeth II to be given to extraordinary people who make Canada proud—for their work of establishing the Calgary Urban Project Society. The Calgary Urban Project Society became the model across all Canada for helping those most in need (many of them homeless) by providing health care, education and housing—all this long before the concept of holistic treatment or an integrated approach engaging mind, body and spirit was part of the common literacy of health professionals. This, to be noted, was accomplished by the Biebers while on an extended furlough while their children finished high school—an interregnum before the two headed back to the South China Seas to fulfill their lifetime calling of working with national governments to establish primary health care systems along with improving tertiary systems in the countries where they landed.
Bieber writes, “Author Brian Palmer even queries the reliability of the mission doctors, who work in adverse and under-resourced conditions. The lack of trust seems to be justifiable, he infers, because they rarely publish their accomplishments in the ivory towers of academia! When they explain to patients they are motivated by the love of Jesus rather than financial gain, somehow that is ‘proselytizing.’ Would it be nobler, I wonder, if doctors were to tell them that the danger pay was good or that they desire adventure or fame? These are unproductive and unfounded arguments by critics who clearly have their own axes to grind, and at a time when the world crisis calls for everyone to roll up their sleeves and get to work in solving the problems facing us all.
“Surely the relief and development organizations that are out there in the world can come to the same conclusion on this one thing—everybody is needed in order to fight diseases such as Ebola, HIV/AIDS or tuberculosis; every agency has strengths that will add to the synergy of the whole. Whether faith-based, local and national government or secular NGO, all have been trained in similar techniques and scientific method. Collaboration is what is needed in order for groups that are stronger to support those that are less resourced to achieve a common goal.”
To be fair, the Slate journalist admits to being conflicted. After listing the flaws of medical mission approaches, Palmer writes, “And yet, truth be told, these valid critiques don’t fully explain my discomfort with missionary medicine. If we had thousands of secular doctors doing exactly the same work, I would probably excuse most of these flaws. ‘They’re doing work no one else will,’ I would say. ‘You can’t expect perfection.’ ”
At least he admits to bias. Knowing my share of medical missionaries, many of whom I consider truly heroic and who are radicalizing the health care systems of the countries in which they serve for the undeniable betterment of those societies, Palmer’s approach seems a tad unprofessional as far as journalism goes. He concludes, “As an atheist, I try to make choices based on evidence and reason. So until we’re finally ready to invest heavily in secular medicine for Africa, I suggest we stand aside and let God do His work.”
A deeper search in PubMed, driven admittedly by my own bias, led me to the excellent data-informed article utilizing research on the topic from both the scientific, theological and academic sectors by Jeff Levin, titled “Partnerships between the faith-based and medical sectors: Implications for preventive medicine and public health.”
Levin concludes with a quotation that complements his conclusion: “Former U.S. Surgeon General David Satcher, a widely revered public health leader, has made this very point: ‘Through partnership with faith organizations and the use of health promotion and disease-prevention sciences, we can form a mighty alliance to build strong, healthy, and productive communities.’ There is historical precedent for such an alliance, and informed by science and scholarship, it is in our best interest for this to continue and to flourish.”

How many of us in the faith-based sector have wrestled with the theological meaning of health? What is the history of the impact of faith (particularly Christian faith because that is the bias from which I write) on the ongoing movement of medicine in these modern centuries? Why does it matter?
I recently experienced a small snapshot of current industrialized medicine. Last year I underwent a hiatal repair laparoscopic surgery. The best I can ascertain from the Medicare summary notice, which included everything administered the day of the procedure through an overnight stay in the hospital for observation with a release the next day, was the bill.
In addition, I experienced watching a son die at age 41 (Jeremy, the son who accompanied me to Mexico, leaving behind a wife and three small children, then ages 6, 4 and six months), not only from a rare lymphoma that kept him in a superior hospital in Chicago for more than five months but also from the side effects and complications of the aggressive cancer treatments. This all has given me additional perspective on medical approaches.
It Takes Only One Mosquito — to lead to remarkable truths about faith-based organizations and world health: Part 1 | Part 3
This Special Report originally appeared on GFA.org.
Learn more about how Mosquito Nets offer protection for families, saving them from the sickening agony or death from malaria.
Click here, to read more blogs on Patheos from Gospel for Asia.
Learn more about Gospel for Asia: Facebook | YouTube | Instagram | Sourcewatch | Integrity | Lawsuit Update | 5 Distinctives | 6 Remarkable Facts | Media Room | Fighting Malaria | Endorsements | 40th Anniversary | Lawsuit Response |













